|
7/25/2023 0 Comments Hospital incubator baby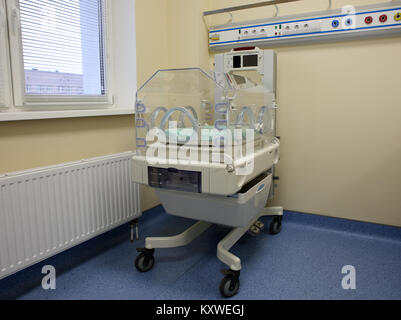
The sensors are strapped gently to your baby’s foot or hand. These monitors check the amount of oxygen in your baby's blood, by shining a light through their skin. Wires run from the pads to the monitoring machine. These monitors pick up these signals through small pads put on your baby’s chest. They can also pick up changes in your baby's breathing. These machines pick up electrical signals given out from your baby’s heart, and always check that it is beating properly. It is the tube which passes the air into your baby's lungs from the ventilator. It is either put in through your baby's nose or mouth. This is put down your baby's windpipe (called a trachea by health professionals) if they are on a ventilator. High-flow is where warm, moist air with or without oxygen (depending on what your baby needs) flows into your baby’s lungs through small tubes in their nose.Įndotracheal (pronounced en-doe-track-eel) tube Some babies need help with their breathing but do not need something as strong as a ventilator. Heated, humidified high-flow nasal cannula (also called 'high-flow' or 'optiflow') This is given through a mask or a small tube in your baby's noce and helps to regulate their breathing. Non-invasic positive pressure ventilations (also called BiPap) CPAP slightly raises the pressure of the air, which helps keep your baby’s lungs inflated. These blow air, with or without oxygen, (depending on what your baby needs) through two thin tubes in your baby’s nose, or through a small mask over their nose. This might look worrying, but it can work very well for some kinds of lung conditions.Ĭontinuous positive airway pressure (often shortened to 'CPAP') Your baby’s chest will look like it is vibrating. High frequency oscillating ventilators: These blow small amounts of air, with or without added oxygen, (depending on what your baby needs) into the lungs very quickly, hundreds of times a minute. This inflates your baby’s lungs and is adjusted depending on what your baby needs. Ventilators: These blow air with or without added oxygen (depending on what your baby needs) gently into your baby’s lungs through a tube which is passed through their nose or mouth. Premature babies' lungs in particular might not be developed enough to manage breathing by themselves yet.ĭepending on what your baby needs, they might be put on a machine called a ventilator – this helps your baby to breathe. If a baby is born prematurely or with a medical condition, they may struggle to breathe by themselves. Once they are born, babies get their oxygen by breathing. The oxygen in the birth parent's blood passes across the placenta and into the umbilical cord (the cord that connects the baby to the placenta and which is cut at birth). Ventilators and breathing machinesīefore your baby was born, they received all the oxygen they needed from their birth parent. 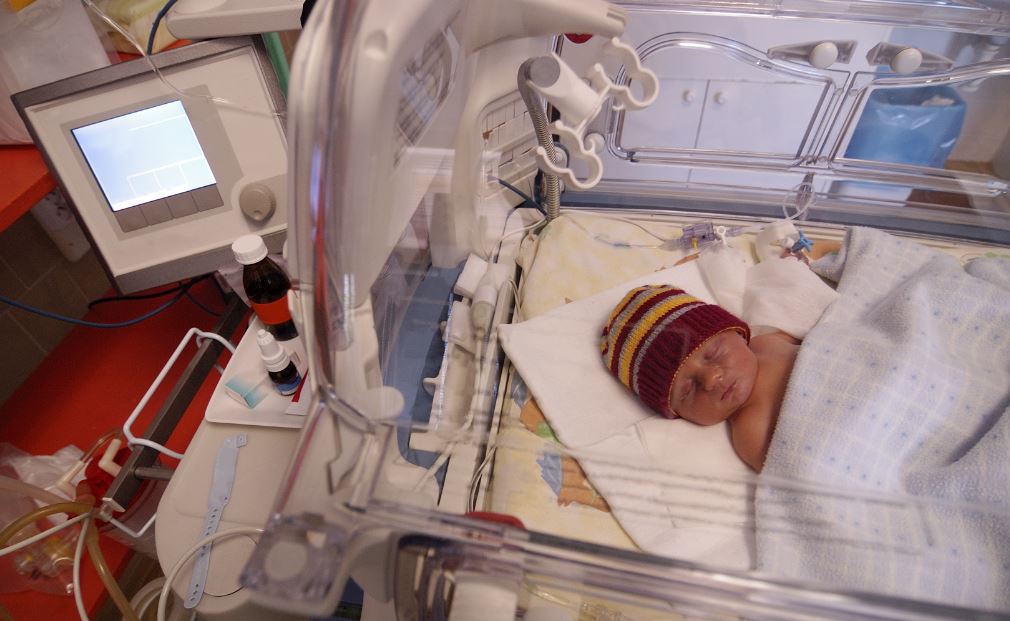
If the sensor falls off or is not working properly, an alarm sounds, and a nurse will check the temperature of the incubator. The temperature is controlled in two ways – either with controls or using an automatic sensor on your baby's skin. Other incubators have open tops and an overhead heater or heated mattresses. This helps keep the heat and humidity in the incubator, stopping too much moisture evaporating from your baby’s fine skin. Some incubators are closed boxes with hand holes on the side. Premature or sick babies can struggle to stay warm on their own. Incubators are clear boxes which help keep your baby warm. Endotracheal intubation in children: practice recommendations, insights, and future directions. Ibarra-Sarlat M, Terrones-Vargas E, Romero- Espinoza L, Castañeda-Muciño G, Herrera-Landero A, Núñez-Enríquez JC. A study of practice behavior for endotracheal intubation site for children with congenital heart disease undergoing surgery: Impact of endotracheal intubation site on perioperative outcomes-an analysis of the Society of Thoracic Surgeons Congenital Cardiac Anesthesia Society database. Greene NH, Jooste EH, Thibault DP, et al. Nasotracheal Intubation. In: Reichman EF. eds. Upper airway tract complications of endotracheal intubation. Intraoperative ventilation and postoperative respiratory assistance. 
Enteral and parenteral nutrition.īall L, Pelosi P. How soon should we start interventional feeding in the ICU?. 
Association of checklist use in endotracheal intubation with clinically important outcomes: A systematic review and meta analysis.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
